Product Development

Chinmay Chandgude
Healthcare App Development Cost in 2026: A Transparent Breakdown by Product Type

Search "healthcare app development cost" and you get estimates ranging from $30,000 to $600,000. Both numbers are correct. The problem is they describe completely different products.
A symptom tracker with no clinical data. A telemedicine platform integrated with Epic and Cerner. A remote patient monitoring system billing Medicare under RPM codes. All three are "healthcare apps." They share almost nothing cost-wise. Collapsing them into a single range is how founders bring a $150K budget to a $280K project.
This article separates them. Seven product types, real cost ranges per type, the five biggest cost drivers quantified in actual dollars, and the hidden line items that consistently blow budgets mid-project. No vague "it depends." Specific enough to bring to a CFO, honest enough to actually help you plan.
Why Healthcare App Development Costs More Than Standard Software
Healthcare app development costs 30–40% more than equivalent non-healthcare software because three factors have no parallel in standard development: mandatory HIPAA compliance architecture, EHR integration with regulated data standards, and clinical-grade QA that must validate patient safety, not just functionality.
The single most useful framing for any healthcare app budget is the IBM 2025 Cost of a Data Breach Report. Healthcare remained the most expensive industry for data breaches for the 14th consecutive year, with an average breach cost of $7.42 million globally and $10.22 million in the United States, both primary findings from the IBM 2025 Cost of a Data Breach report. That is not a scare statistic. It is context for why the compliance and security spend in your budget is insurance, not overhead.
The mechanics of higher cost break down into three areas.
HIPAA compliance is not a feature you add. It is the foundation the entire system is built on: HIPAA-eligible cloud hosting with a signed Business Associate Agreement, database encryption at rest and in transit, role-based access controls, audit logging for every PHI interaction, and vendor governance across every third party in the stack. Building this correctly from the start adds 20–30% to total project budget. Retrofitting it after a hospital partner's security audit or an investor's due diligence review costs 2–3x more, according to analysis from Webkorps.
EHR integration has no equivalent in consumer software. Connecting to Epic, Cerner, or Athenahealth requires understanding proprietary APIs, navigating vendor certification programs, handling HL7 and FHIR data standards, and passing security reviews that take weeks. A single EHR integration typically costs $15,000–$150,000 depending on the depth of connection and the specific vendor.
Clinical QA requires testing layers that standard apps do not need: functional testing, integration testing against live and sandbox EHR environments, security and penetration testing, HIPAA compliance testing, and in some cases clinical validation with actual clinicians reviewing workflows. Together these typically consume 20–30% of total project budget. Budget for it upfront or pay for it as emergency rework after a failed hospital deployment.
Cost by Product Type: The Breakdown
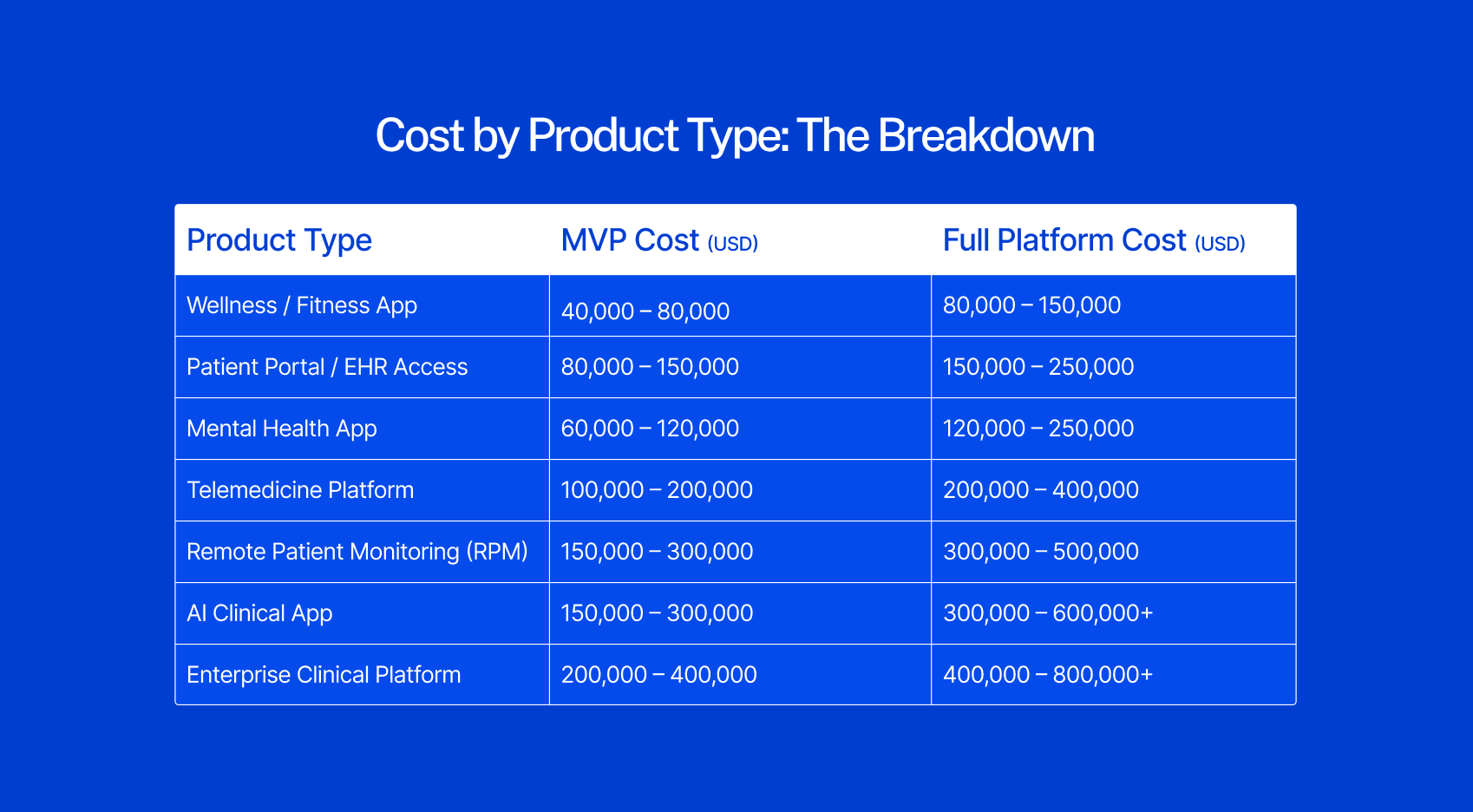
Healthcare app development costs range from $40,000–$80,000 for a wellness or fitness app with no clinical data, to $400,000–$800,000+ for an enterprise clinical platform with multi-EHR integration, AI features, and FDA Software as a Medical Device requirements.
The ranges below reflect 2026 market rates, typical scope for each product type, and what a production-ready MVP versus a full platform includes. They are grounded across multiple cost analysis sources and Latent's own project experience across 100+ healthcare products shipped.
Wellness and Fitness Apps (No PHI)
MVP range: $40,000–$80,000 Full platform: $80,000–$150,000 MVP timeline: 8–16 weeks
These are apps that track activity, nutrition, sleep, stress, or general wellbeing, with no protected health information. No clinical records, no provider connection, no PHI. HIPAA does not apply. That changes the cost profile significantly.
The primary cost drivers are UX (the category lives or dies on user experience), wearable SDK integration (Apple HealthKit, Google Fit, Garmin), notification logic for habit formation, and analytics to understand retention. The moment you add a provider-facing view, medication tracking with prescription data, or lab result access, you cross into PHI territory and the budget tier shifts. Know which category your product is in before you scope.
Internal link: our guide to benefits of mobile health apps covers the evidence base for which features drive clinical outcomes.
Patient-Facing Portal and EHR Access Apps
MVP range: $80,000–$150,000 Full platform: $150,000–$250,000 MVP timeline: 12–20 weeks
Apps that give patients access to their medical records, lab results, appointment scheduling, and provider messaging. This is the fastest-growing category by adoption: 57% of US individuals used smartphone-based medical record access in 2024, up from 38% in 2020 (ASTP/ONC HINTS 7).
FHIR R4 integration is the core cost driver. Under the 21st Century Cures Act, certified health IT must support FHIR R4 APIs, so any app connecting to EHR records must build against this standard. A read-only FHIR connection starts at $15,000–$25,000. The full HIPAA compliance layer adds another $15,000–$40,000. The MVP includes patient authentication, read-only record access, appointment viewing, and secure messaging. Later phases add prescription management, bill payment, family account support, and bidirectional data sync.
Mental Health and Behavioral Health Apps
MVP range: $60,000–$120,000 Full platform: $120,000–$250,000 MVP timeline: 10–18 weeks
The fastest-growing category by user demand. The cost range is wide because of a single architecture decision that must be made before writing a line of code: is this a wellness app making no clinical claims, or a prescription digital therapeutic (PDT) making treatment claims?
Wellness apps (meditation, CBT exercises, mood tracking without clinical claims) require HIPAA compliance but not FDA clearance. PDTs claiming to treat a diagnosed condition require FDA Software as a Medical Device (SaMD) clearance, which adds 6–12 months and $200,000–$500,000 to the project. Our guide to Software as a Medical Device covers the classification decision in detail. Choosing wrong costs more in both time and money than making the call correctly upfront.
Telemedicine Platforms
MVP range: $100,000–$200,000 Full platform: $200,000–$400,000 MVP timeline: 14–24 weeks
Telemedicine carries the highest compliance load of any category outside regulated medical devices: HIPAA, multi-state licensing for providers, PCI compliance for payments, and real-time infrastructure that standard apps do not need. The provider-facing side consistently consumes more development time than the patient side, scheduling, documentation, queue management, and clinical workflow integration are more complex than they look.
The real-time video layer is its own budget line. Do not build video infrastructure from scratch. Twilio and Vonage both offer HIPAA-eligible video SDKs. The integration and compliance hardening still costs $30,000–$50,000, but it is a fraction of custom build cost. MVP includes secure video consultation, appointment scheduling, basic provider profile, and payment. E-prescribing, EHR write-back, and multi-provider support are Phase 2.
For a detailed scope breakdown, see our guide to telemedicine platform development.
Remote Patient Monitoring (RPM) Platforms
MVP range: $150,000–$300,000 Full platform: $300,000–$500,000 MVP timeline: 16–28 weeks
RPM is the category with the clearest path to reimbursement. Medicare CPT codes 99453, 99454, 99457, and 99458 created a billing pathway that most mHealth categories lack. When a product connects to Medicare billing, adoption becomes a financial decision for providers rather than a patient engagement experiment.
The cost is driven by three layers that do not exist in other categories: device connectivity (each wearable or connected device requires its own SDK integration and certification); real-time alert logic (vitals thresholds must trigger provider alerts within defined time windows, which requires event-driven backend architecture); and provider-facing dashboards with billing documentation outputs. 80% of US hospitals already use wearables for RPM, the software layer connecting device data to clinical workflows is the gap being built into.
For the device ecosystem context, see our guide to top remote patient monitoring devices.
AI-Powered Clinical Apps (Diagnostics, Decision Support, Triage)
MVP range: $150,000–$300,000 Full platform: $300,000–$600,000+ MVP timeline: 16–32 weeks
AI features that influence clinical decisions almost always land in FDA SaMD territory. Diagnostic support, risk stratification, triage algorithms, and imaging analysis all require FDA clearance before you can ship and charge. That adds 6–12 months and $50,000–$150,000 in regulatory work on top of development costs.
AI models in clinical apps also carry data governance costs that consumer AI does not: training data must be de-identified, model validation requires clinical evidence, and inference logging is required for audit purposes. The most common budget mistake in this category is scoping the AI features without scoping the regulatory pathway, discovering FDA requirements mid-development when the architecture is already set.
Enterprise Clinical Platforms (EHR, EMR, Hospital Management)
MVP range: $200,000–$400,000 Full platform: $400,000–$800,000+ MVP timeline: 20–40 weeks
Multi-department systems, custom EHR builds for specialty practices, and hospital management platforms are enterprise products. They are priced as enterprise products. A single-specialty custom EMR for a nephrology or oncology practice with one EHR integration typically lands $200,000–$400,000. Multi-EHR integration covering Epic, Cerner, and a regional system can push bidirectional integration costs alone past $300,000.
These products require clinical validation at every stage: actual physicians and nurses reviewing workflows, finding edge cases, and signing off on clinical logic. Budget 40–80 hours of senior clinical staff time per major review cycle. That is not a vendor invoice, but it is a real project cost.
The Five Biggest Cost Drivers: Quantified
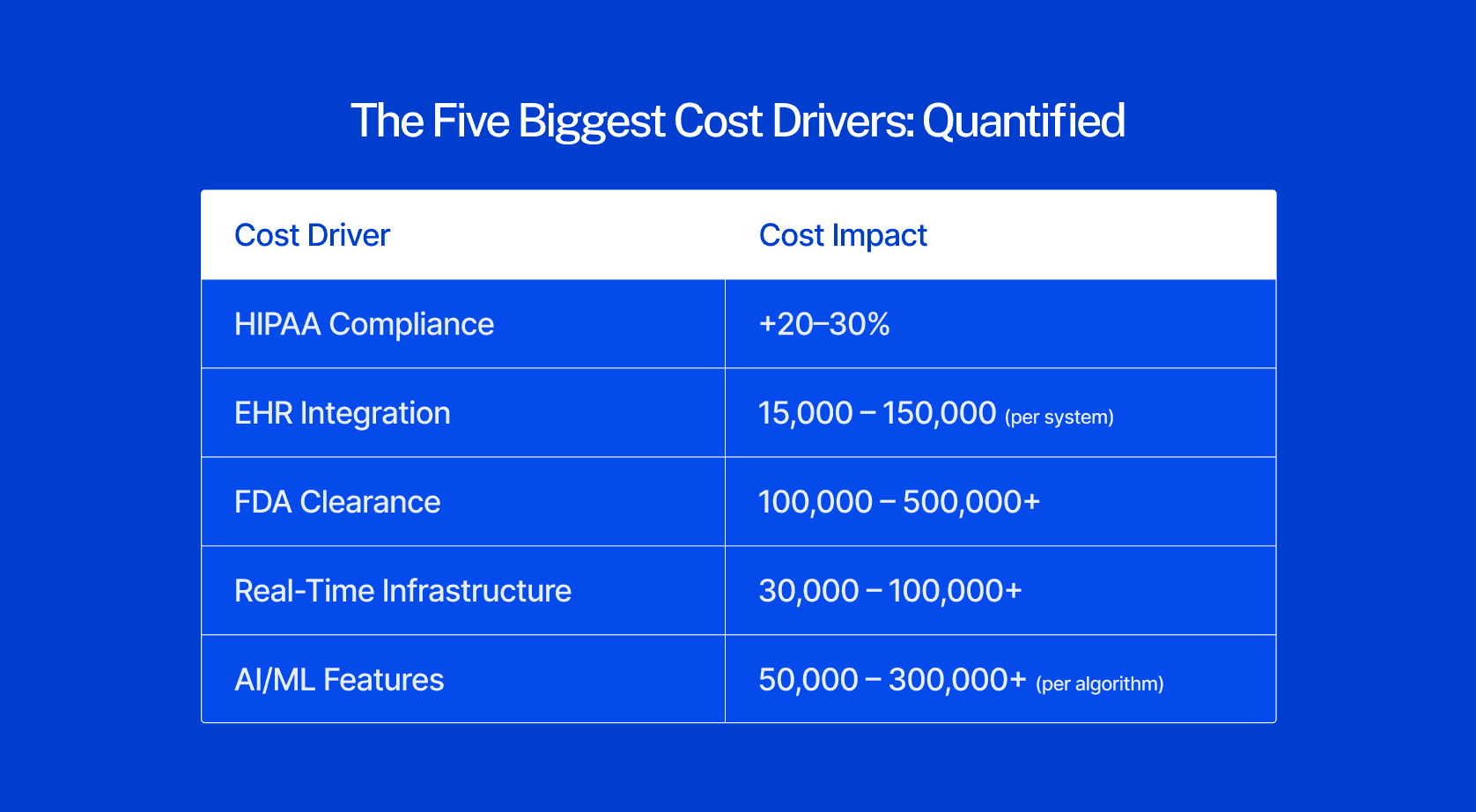
The five factors that most significantly drive healthcare app development cost are HIPAA compliance architecture (20–30% of total budget), EHR integration scope ($15K–$150K per system), team composition ($50–$250/hr variance by region and experience), platform choice (native vs cross-platform saves 30%), and real-time infrastructure for video and monitoring ($30K–$80K added cost).
1. HIPAA Compliance Architecture: 20–30% of Total Budget
Every app that creates, receives, stores, or transmits protected health information in the US needs:
HIPAA-eligible cloud hosting (AWS, Azure, or Google Cloud with a signed BAA)
Database encryption at rest and in transit (AES-256 is the standard)
Role-based access controls with minimum necessary access enforcement
Full audit logging for every PHI interaction
Business Associate Agreements with every vendor in the stack
Documented risk analysis and risk management processes
This infrastructure layer typically adds $15,000–$75,000 to project cost depending on app complexity. Built correctly from the start, it is a one-time cost. Retrofitted after a hospital partner's vendor security questionnaire arrives, the same work costs 2–3x more, plus the cost of the delay.
Our guide to HIPAA-compliant app development covers the specific architecture requirements and what each one means for your stack.
2. EHR Integration: $15K–$150K Per System
This is the single most expensive individual line item in most clinical healthcare apps, and the most frequently underestimated. The cost depends on four variables:
Read-only vs bidirectional. Pulling patient data into your app (read-only FHIR) starts at $15,000–$25,000 per EHR system. Writing clinical notes, vitals, or assessment results back to the EHR (bidirectional) starts at $50,000–$80,000 per system. The write path requires clinical validation of every data element you push, vendor certification review, and extensive testing against live EHR environments.
Which EHR vendor. Epic is the most expensive to integrate ($18,000–$80,000) due to App Orchard and Connection Hub certification requirements. Athenahealth is typically the least expensive ($10,000–$48,000) because of its API-first architecture. Cerner sits between them. These figures come from the Taction Software EHR Integration Cost Guide 2026.
Number of systems. Multi-system integration covering Epic, Cerner, and a regional system can push total integration costs past $150,000–$300,000. Each system requires separate certification, sandbox access, testing, and ongoing maintenance.
Protocol choice. FHIR integrations cost more upfront but are easier to maintain and more portable across systems. HL7v2 integrations are cheaper initially but require more custom transformation logic and generate higher maintenance costs over time.
For the full technical breakdown, see our guide to FHIR integration for healthcare apps.
3. Team Composition and Geography: $50–$250/hr Variance
US-based senior healthcare developers: $150–$250/hr. Eastern Europe and India senior healthcare developers: $50–$100/hr. For a 2,000-hour project, the rate difference is $200,000–$300,000. That looks like an obvious decision until you factor in domain experience.
A team without prior HIPAA implementation experience spends 30–40% more time on compliance architecture than a team that has built compliant systems before. A developer encountering HL7v2 message formats for the first time takes three times longer to build a working EHR integration than one who has done it, according to analysis from Interexy. The savings from lower hourly rates disappear entirely in additional hours and rework cycles.
The right evaluation is not hourly rate. It is: has this team built HIPAA-compliant apps before? Have they integrated with the specific EHR system on your list? Do they have active developer program memberships with Epic or Cerner that eliminate certification queue time? Those questions determine actual total cost far more than the rate card.
4. Platform Choice: Native vs Cross-Platform Saves 30%
Building separate native iOS and Android apps costs roughly 1.8x a single-platform build. Cross-platform frameworks (Flutter, React Native) share a single codebase across both platforms, saving 30–40% for most patient-facing healthcare apps.
Cross-platform is the right choice for 80% of healthcare apps: patient portals, telemedicine interfaces, wellness apps, medication management, RPM patient-facing apps. Choose native when you need low-level hardware access: direct Bluetooth stack communication for medical device connectivity, biometric authentication beyond what standard SDKs expose, or maximum performance for imaging applications.
The common mistake is defaulting to native "because it is better" without evaluating what the additional 80% cost buys you in your specific use case.
5. Real-Time Infrastructure: $30K–$80K Added Cost
Any feature involving live data, telemedicine video, RPM vitals alerts, real-time secure messaging, live monitoring dashboards, requires backend infrastructure that standard request-response apps do not need:
WebSocket or server-sent event connections for live data streams
Event-driven architecture for alert triggering (vitals breach thresholds)
HIPAA-eligible video infrastructure (Twilio, Vonage, not Zoom)
Load testing and performance validation under concurrent user scenarios
Higher-tier cloud infrastructure with lower latency requirements
This is not a feature cost that shows up on one line of your scope document. It is an infrastructure investment that affects your database architecture, your DevOps setup, your cloud tier, and your QA strategy. Budget $30,000–$80,000 for a real-time layer, separate from feature development costs.
Hidden Costs That Blow Budgets Mid-Project
The four hidden costs that most frequently cause healthcare app budgets to overrun are annual penetration testing ($15K–$40K), legal review of BAAs and privacy documentation ($5K–$20K), EHR vendor certification queues that add weeks without warning, and clinical staff validation time that never appears on a vendor invoice but is a real organizational cost.
Annual penetration testing. Any clinical app sold to hospital systems or enterprise health plans requires independent penetration testing from a certified third-party auditor. The cost runs $15,000–$40,000 per engagement. Some hospital procurement contracts require quarterly testing. This is not optional and it is not in the initial build scope, it is an ongoing operating cost that must be in your year-one budget.
Legal review. Business Associate Agreements, Terms of Service, Privacy Policies, patient consent forms, and state-specific telehealth compliance documents all require legal review from healthcare-specialized attorneys. Healthcare legal specialists charge $300–$600/hr. Budget $5,000–$20,000 for initial legal work, more if you are operating across multiple states with varying telehealth regulations.
EHR vendor certification queues. Epic's App Orchard and Connection Hub review processes run 4–8 weeks. Cerner's review process has its own queue. These timelines are not under your control and they are not in your vendor's estimate. If you do not book sandbox access and certification reviews during the discovery phase, you discover the queue mid-project while your sprint velocity has already been planned against a timeline that assumed no wait.
Clinical staff validation time. Your physicians, nurses, or clinical informatics team will spend time reviewing workflows, testing edge cases, and providing feedback on clinical logic. This typically runs 40–80 hours of senior clinical staff time per major review cycle. It does not appear on anyone's invoice. But it is real time with real opportunity cost, and any project that assumes clinical validation "happens automatically" underestimates the coordination and scheduling involved.
The example that plays out repeatedly: a project scoped at $175,000 reaches $265,000 because the EHR certification added eight weeks of idle time billed at maintenance rates, the penetration test was not in the budget, legal review ran $18,000 for a three-state telehealth product, and one round of clinical validation feedback required three sprint revisions to the care plan workflow.
How to Phase Your Build to Control Cost
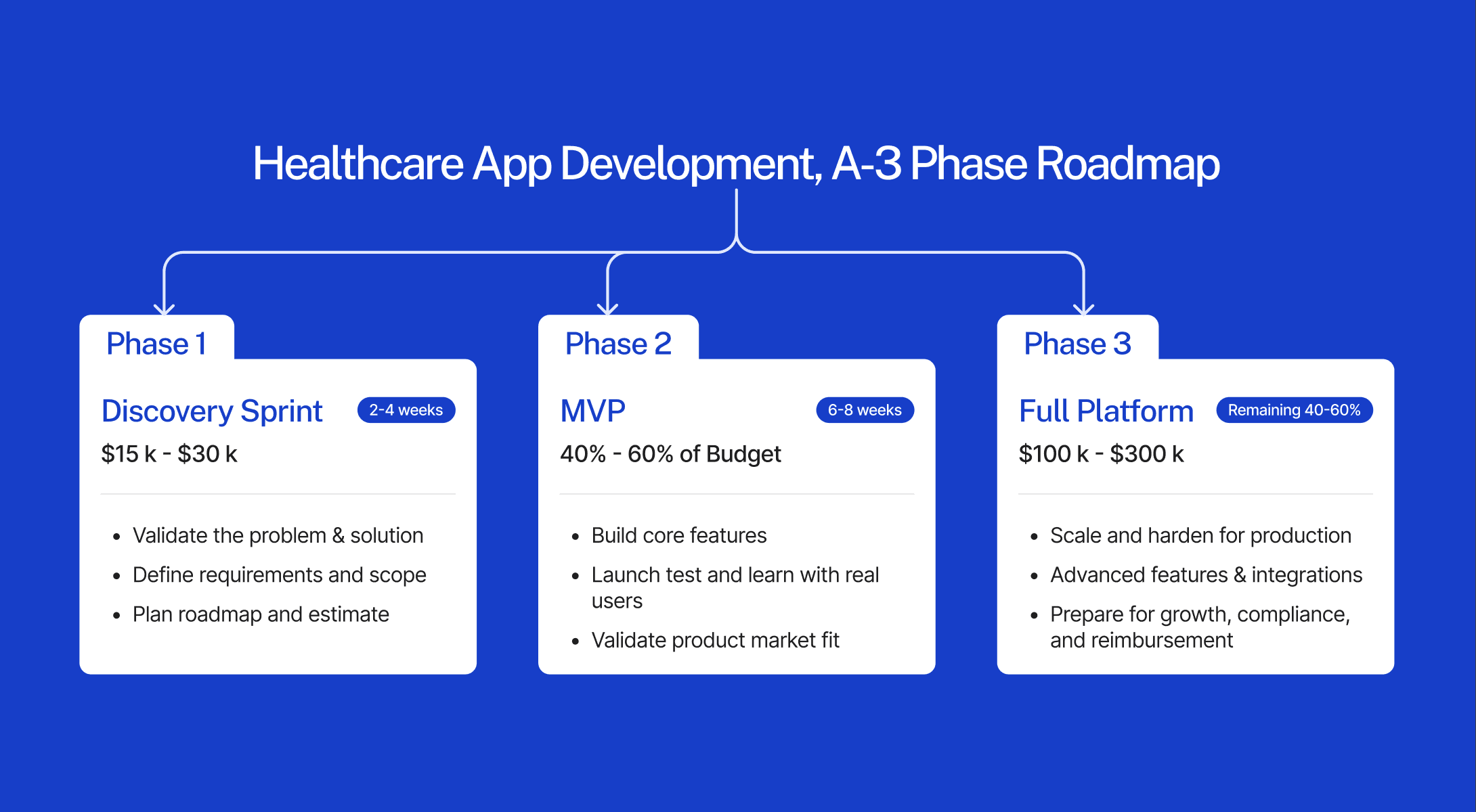
The correct phasing for a healthcare app is: a paid discovery sprint to define compliance architecture and EHR integration scope (2–4 weeks, $15,000–$30,000), followed by an MVP covering the single core clinical workflow with HIPAA infrastructure in place (8–16 weeks, 40–60% of total budget), then Phase 2 adding integrations, secondary workflows, and advanced features.
The discovery sprint is not optional for healthcare. Architecture decisions made in the first four weeks of a project determine approximately 70% of total cost, according to Webkorps' AI healthcare app cost analysis. A proper discovery phase identifies $30,000–$100,000 in scope changes before they become $90,000–$300,000 mid-project rework items. The cost of discovery is always less than the cost of the architecture decisions it prevents.
The healthcare MVP definition differs from consumer app MVP. A healthcare MVP must include the full HIPAA compliance layer and at least read-only EHR access from sprint one. Stripping those as "Phase 2" is how budgets double: the compliance retrofit and EHR integration performed after the rest of the system is built is significantly more expensive than building them in.
Phase 1 (MVP): One core clinical workflow. Full HIPAA infrastructure. One EHR integration (read-only). Basic provider and patient UI. Core notification system. 40–60% of total budget.
Phase 2: Second EHR system. Bidirectional write-back. Advanced analytics. Secondary workflows. AI features if required. Remaining 40–60%.
Budget rule of thumb: add 25% contingency on your first clinical app build. If you have never integrated with the specific EHR vendor on your list, add another 15%.
For the full build process from concept to launch, see our guide to launching a healthtech app in under 90 days and our step-by-step guide to how to develop a healthcare app.
How to Build Without Cutting Compliance
The three most effective ways to reduce healthcare app development cost without compromising compliance are using established HIPAA-eligible third-party infrastructure instead of building it, choosing cross-platform over native for patient-facing apps, and working with a team that has existing EHR vendor developer relationships and certifications.
Do not build what already exists compliantly. Twilio and Vonage for HIPAA-eligible video. Stripe for healthcare payment processing. Auth0 or Okta for identity management and MFA. AWS or Azure for HIPAA-eligible hosting. These are not shortcuts, they are the industry standard. Using them instead of custom-building saves $40,000–$100,000 and eliminates the compliance risk of an untested custom implementation.
Choose cross-platform over native for any app where deep device hardware access is not required. For most patient-facing healthcare apps, it saves 30%.
Team experience with your specific EHR vendor matters more than hourly rate. A team with active Epic Connection Hub membership and prior certification history eliminates 4–8 weeks of queue time. At $80–$150/hr blended rate, that is $25,000–$60,000 in avoided delay cost.
One of the most common false economies is choosing staff augmentation over a managed team for clinical builds. Individual augmented developers do not produce HIPAA compliance documentation, sprint compliance logs, or architecture decision records as default outputs of their work. A managed pod builds these into the operating rhythm of every sprint. Our guide to what is a managed development team explains the ownership difference.
If you are evaluating whether to build in-house or partner, our guide to outsourcing healthcare product development covers the governance and accountability decisions involved.
Latent builds healthcare apps using managed pods, with HIPAA compliance, FHIR architecture, and sprint compliance documentation built in from day one. MVPs in 8–14 weeks, 100+ products shipped across 14 countries. Book a free 30-minute discovery call to get a realistic estimate for your specific product type.
Annual Operating Costs After Launch
Annual operating costs for a clinical healthcare app run 15–25% of initial development cost for maintenance, plus $5,000–$50,000/year for HIPAA-eligible cloud hosting, $15,000–$40,000 for annual penetration testing, and third-party API subscription fees. A $200,000 build typically costs $60,000–$100,000 per year to operate correctly.
Maintenance at 15–25% of build cost covers: security patches (critical for any app with PHI), OS updates (Apple and Google release major iOS/Android updates twice yearly and deprecate APIs), new device SDK versions for wearable integrations, EHR API version updates as vendors evolve their FHIR implementations, and compliance documentation updates as regulations change. This is not optional for clinical apps. An app that skips a security patch cycle is not just a technical liability, it is a HIPAA liability.
Cloud hosting on HIPAA-eligible infrastructure runs $500–$5,000/month depending on user load, data storage volume, and real-time infrastructure requirements. Standard cloud tiers do not include the BAA required for PHI. HIPAA-eligible tiers cost more and must be selected and configured deliberately.
Third-party API fees add up: Twilio video charges per minute of video, EHR marketplace fees apply if you list in Epic's App Orchard or Oracle's marketplace, analytics platforms charge by monthly active user. Budget $500–$5,000/month depending on usage patterns.
Total cost of ownership for a $200,000 clinical app: development ($200K) + Year 1 operating costs ($70K–$100K) + ongoing annual costs ($60K–$100K/year). This needs to be in the business case at the start, not discovered during the first budget review after launch.
What It Actually Costs to Build Secure and Right the First Time
The question framed wrong is: "What is the cheapest path to launch?"
The question framed right is: "What is the cost of a healthcare data breach ($10.22M US average in 2025), a failed hospital procurement process because compliance documentation was missing, or a six-sprint compliance retrofit, versus building it correctly in the first place?"
The teams that consistently bring healthcare products to market on budget are the ones that front-loaded the decisions: compliance architecture in discovery, EHR integration vendor relationships secured before development starts, and a team with prior experience on both. The teams that consistently double their budgets are the ones that deferred those decisions because the initial estimate looked cleaner without them.
Latent builds healthcare products using managed execution pods, cross-functional teams that own delivery from sprint planning through deployment, with HIPAA compliance, FHIR architecture, and IP documentation built into the operating rhythm from day one. We have shipped 100+ products across 14 countries, including telemedicine platforms, RPM systems, clinical apps, and patient engagement tools.
If you are scoping a healthcare app build and need a realistic, product-specific cost estimate, book a free 30-minute discovery call. We will map your product type, your compliance requirements, your EHR integration list, and give you a defensible budget range before you commit to anything.
Or start with a free 2-week discovery sprint: we scope the architecture, define the compliance path, and produce a full technical specification before your first dollar of development spend. Book your discovery sprint.
Frequently Asked Questions
How much does it cost to build a healthcare app in 2026?
Healthcare app development cost in 2026 ranges from $40,000–$80,000 for a wellness or fitness app with no clinical data, $80,000–$150,000 for a patient-facing portal with EHR access, $100,000–$200,000 for a telemedicine platform MVP, $150,000–$300,000 for a remote patient monitoring platform, $150,000–$300,000 for an AI clinical app MVP, and $200,000–$400,000+ for an enterprise clinical platform. The range is wide because the products are fundamentally different. A wellness tracker and a multi-EHR telemedicine platform share almost nothing cost-wise.
What is the most expensive part of healthcare app development?
EHR integration and HIPAA compliance architecture together typically account for 35–50% of total budget in clinical apps. A single EHR integration (read-only FHIR) starts at $15,000–$25,000; bidirectional integration with Epic starts at $50,000–$80,000. HIPAA compliance adds 20–30% to total budget. These two line items alone often exceed the total budget that founders initially allocate for the entire project.
How much does HIPAA compliance add to app development cost?
HIPAA compliance architecture adds 20–30% to total development budget when built correctly from the start: typically $15,000–$75,000 depending on app complexity. This covers HIPAA-eligible hosting, encryption, audit logging, access controls, and BAA management. Retrofitting HIPAA compliance after launch costs 2–3x more than building it in from the start, plus the risk exposure during the gap.
How long does it take to build a healthcare app?
Typical timelines for a production-ready MVP: wellness app 8–16 weeks, patient portal 12–20 weeks, mental health app 10–18 weeks, telemedicine platform 14–24 weeks, RPM platform 16–28 weeks, AI clinical app 16–32 weeks, enterprise clinical platform 20–40 weeks. These timelines assume the discovery sprint has been completed and EHR vendor sandbox access has been secured before development starts. Missing either adds weeks regardless of team velocity.
What are the annual operating costs for a healthcare app?
Annual operating costs for a clinical healthcare app run 15–25% of initial development cost for maintenance and updates, plus HIPAA-eligible cloud hosting ($500–$5,000/month), annual penetration testing ($15,000–$40,000), and third-party API fees ($500–$5,000/month depending on usage). A $200,000 build typically costs $60,000–$100,000 per year to operate correctly. This figure must be in the business case from the start, not discovered after launch.
Search "healthcare app development cost" and you get estimates ranging from $30,000 to $600,000. Both numbers are correct. The problem is they describe completely different products.
A symptom tracker with no clinical data. A telemedicine platform integrated with Epic and Cerner. A remote patient monitoring system billing Medicare under RPM codes. All three are "healthcare apps." They share almost nothing cost-wise. Collapsing them into a single range is how founders bring a $150K budget to a $280K project.
This article separates them. Seven product types, real cost ranges per type, the five biggest cost drivers quantified in actual dollars, and the hidden line items that consistently blow budgets mid-project. No vague "it depends." Specific enough to bring to a CFO, honest enough to actually help you plan.
Why Healthcare App Development Costs More Than Standard Software
Healthcare app development costs 30–40% more than equivalent non-healthcare software because three factors have no parallel in standard development: mandatory HIPAA compliance architecture, EHR integration with regulated data standards, and clinical-grade QA that must validate patient safety, not just functionality.
The single most useful framing for any healthcare app budget is the IBM 2025 Cost of a Data Breach Report. Healthcare remained the most expensive industry for data breaches for the 14th consecutive year, with an average breach cost of $7.42 million globally and $10.22 million in the United States, both primary findings from the IBM 2025 Cost of a Data Breach report. That is not a scare statistic. It is context for why the compliance and security spend in your budget is insurance, not overhead.
The mechanics of higher cost break down into three areas.
HIPAA compliance is not a feature you add. It is the foundation the entire system is built on: HIPAA-eligible cloud hosting with a signed Business Associate Agreement, database encryption at rest and in transit, role-based access controls, audit logging for every PHI interaction, and vendor governance across every third party in the stack. Building this correctly from the start adds 20–30% to total project budget. Retrofitting it after a hospital partner's security audit or an investor's due diligence review costs 2–3x more, according to analysis from Webkorps.
EHR integration has no equivalent in consumer software. Connecting to Epic, Cerner, or Athenahealth requires understanding proprietary APIs, navigating vendor certification programs, handling HL7 and FHIR data standards, and passing security reviews that take weeks. A single EHR integration typically costs $15,000–$150,000 depending on the depth of connection and the specific vendor.
Clinical QA requires testing layers that standard apps do not need: functional testing, integration testing against live and sandbox EHR environments, security and penetration testing, HIPAA compliance testing, and in some cases clinical validation with actual clinicians reviewing workflows. Together these typically consume 20–30% of total project budget. Budget for it upfront or pay for it as emergency rework after a failed hospital deployment.
Cost by Product Type: The Breakdown

Healthcare app development costs range from $40,000–$80,000 for a wellness or fitness app with no clinical data, to $400,000–$800,000+ for an enterprise clinical platform with multi-EHR integration, AI features, and FDA Software as a Medical Device requirements.
The ranges below reflect 2026 market rates, typical scope for each product type, and what a production-ready MVP versus a full platform includes. They are grounded across multiple cost analysis sources and Latent's own project experience across 100+ healthcare products shipped.
Wellness and Fitness Apps (No PHI)
MVP range: $40,000–$80,000 Full platform: $80,000–$150,000 MVP timeline: 8–16 weeks
These are apps that track activity, nutrition, sleep, stress, or general wellbeing, with no protected health information. No clinical records, no provider connection, no PHI. HIPAA does not apply. That changes the cost profile significantly.
The primary cost drivers are UX (the category lives or dies on user experience), wearable SDK integration (Apple HealthKit, Google Fit, Garmin), notification logic for habit formation, and analytics to understand retention. The moment you add a provider-facing view, medication tracking with prescription data, or lab result access, you cross into PHI territory and the budget tier shifts. Know which category your product is in before you scope.
Internal link: our guide to benefits of mobile health apps covers the evidence base for which features drive clinical outcomes.
Patient-Facing Portal and EHR Access Apps
MVP range: $80,000–$150,000 Full platform: $150,000–$250,000 MVP timeline: 12–20 weeks
Apps that give patients access to their medical records, lab results, appointment scheduling, and provider messaging. This is the fastest-growing category by adoption: 57% of US individuals used smartphone-based medical record access in 2024, up from 38% in 2020 (ASTP/ONC HINTS 7).
FHIR R4 integration is the core cost driver. Under the 21st Century Cures Act, certified health IT must support FHIR R4 APIs, so any app connecting to EHR records must build against this standard. A read-only FHIR connection starts at $15,000–$25,000. The full HIPAA compliance layer adds another $15,000–$40,000. The MVP includes patient authentication, read-only record access, appointment viewing, and secure messaging. Later phases add prescription management, bill payment, family account support, and bidirectional data sync.
Mental Health and Behavioral Health Apps
MVP range: $60,000–$120,000 Full platform: $120,000–$250,000 MVP timeline: 10–18 weeks
The fastest-growing category by user demand. The cost range is wide because of a single architecture decision that must be made before writing a line of code: is this a wellness app making no clinical claims, or a prescription digital therapeutic (PDT) making treatment claims?
Wellness apps (meditation, CBT exercises, mood tracking without clinical claims) require HIPAA compliance but not FDA clearance. PDTs claiming to treat a diagnosed condition require FDA Software as a Medical Device (SaMD) clearance, which adds 6–12 months and $200,000–$500,000 to the project. Our guide to Software as a Medical Device covers the classification decision in detail. Choosing wrong costs more in both time and money than making the call correctly upfront.
Telemedicine Platforms
MVP range: $100,000–$200,000 Full platform: $200,000–$400,000 MVP timeline: 14–24 weeks
Telemedicine carries the highest compliance load of any category outside regulated medical devices: HIPAA, multi-state licensing for providers, PCI compliance for payments, and real-time infrastructure that standard apps do not need. The provider-facing side consistently consumes more development time than the patient side, scheduling, documentation, queue management, and clinical workflow integration are more complex than they look.
The real-time video layer is its own budget line. Do not build video infrastructure from scratch. Twilio and Vonage both offer HIPAA-eligible video SDKs. The integration and compliance hardening still costs $30,000–$50,000, but it is a fraction of custom build cost. MVP includes secure video consultation, appointment scheduling, basic provider profile, and payment. E-prescribing, EHR write-back, and multi-provider support are Phase 2.
For a detailed scope breakdown, see our guide to telemedicine platform development.
Remote Patient Monitoring (RPM) Platforms
MVP range: $150,000–$300,000 Full platform: $300,000–$500,000 MVP timeline: 16–28 weeks
RPM is the category with the clearest path to reimbursement. Medicare CPT codes 99453, 99454, 99457, and 99458 created a billing pathway that most mHealth categories lack. When a product connects to Medicare billing, adoption becomes a financial decision for providers rather than a patient engagement experiment.
The cost is driven by three layers that do not exist in other categories: device connectivity (each wearable or connected device requires its own SDK integration and certification); real-time alert logic (vitals thresholds must trigger provider alerts within defined time windows, which requires event-driven backend architecture); and provider-facing dashboards with billing documentation outputs. 80% of US hospitals already use wearables for RPM, the software layer connecting device data to clinical workflows is the gap being built into.
For the device ecosystem context, see our guide to top remote patient monitoring devices.
AI-Powered Clinical Apps (Diagnostics, Decision Support, Triage)
MVP range: $150,000–$300,000 Full platform: $300,000–$600,000+ MVP timeline: 16–32 weeks
AI features that influence clinical decisions almost always land in FDA SaMD territory. Diagnostic support, risk stratification, triage algorithms, and imaging analysis all require FDA clearance before you can ship and charge. That adds 6–12 months and $50,000–$150,000 in regulatory work on top of development costs.
AI models in clinical apps also carry data governance costs that consumer AI does not: training data must be de-identified, model validation requires clinical evidence, and inference logging is required for audit purposes. The most common budget mistake in this category is scoping the AI features without scoping the regulatory pathway, discovering FDA requirements mid-development when the architecture is already set.
Enterprise Clinical Platforms (EHR, EMR, Hospital Management)
MVP range: $200,000–$400,000 Full platform: $400,000–$800,000+ MVP timeline: 20–40 weeks
Multi-department systems, custom EHR builds for specialty practices, and hospital management platforms are enterprise products. They are priced as enterprise products. A single-specialty custom EMR for a nephrology or oncology practice with one EHR integration typically lands $200,000–$400,000. Multi-EHR integration covering Epic, Cerner, and a regional system can push bidirectional integration costs alone past $300,000.
These products require clinical validation at every stage: actual physicians and nurses reviewing workflows, finding edge cases, and signing off on clinical logic. Budget 40–80 hours of senior clinical staff time per major review cycle. That is not a vendor invoice, but it is a real project cost.
The Five Biggest Cost Drivers: Quantified

The five factors that most significantly drive healthcare app development cost are HIPAA compliance architecture (20–30% of total budget), EHR integration scope ($15K–$150K per system), team composition ($50–$250/hr variance by region and experience), platform choice (native vs cross-platform saves 30%), and real-time infrastructure for video and monitoring ($30K–$80K added cost).
1. HIPAA Compliance Architecture: 20–30% of Total Budget
Every app that creates, receives, stores, or transmits protected health information in the US needs:
HIPAA-eligible cloud hosting (AWS, Azure, or Google Cloud with a signed BAA)
Database encryption at rest and in transit (AES-256 is the standard)
Role-based access controls with minimum necessary access enforcement
Full audit logging for every PHI interaction
Business Associate Agreements with every vendor in the stack
Documented risk analysis and risk management processes
This infrastructure layer typically adds $15,000–$75,000 to project cost depending on app complexity. Built correctly from the start, it is a one-time cost. Retrofitted after a hospital partner's vendor security questionnaire arrives, the same work costs 2–3x more, plus the cost of the delay.
Our guide to HIPAA-compliant app development covers the specific architecture requirements and what each one means for your stack.
2. EHR Integration: $15K–$150K Per System
This is the single most expensive individual line item in most clinical healthcare apps, and the most frequently underestimated. The cost depends on four variables:
Read-only vs bidirectional. Pulling patient data into your app (read-only FHIR) starts at $15,000–$25,000 per EHR system. Writing clinical notes, vitals, or assessment results back to the EHR (bidirectional) starts at $50,000–$80,000 per system. The write path requires clinical validation of every data element you push, vendor certification review, and extensive testing against live EHR environments.
Which EHR vendor. Epic is the most expensive to integrate ($18,000–$80,000) due to App Orchard and Connection Hub certification requirements. Athenahealth is typically the least expensive ($10,000–$48,000) because of its API-first architecture. Cerner sits between them. These figures come from the Taction Software EHR Integration Cost Guide 2026.
Number of systems. Multi-system integration covering Epic, Cerner, and a regional system can push total integration costs past $150,000–$300,000. Each system requires separate certification, sandbox access, testing, and ongoing maintenance.
Protocol choice. FHIR integrations cost more upfront but are easier to maintain and more portable across systems. HL7v2 integrations are cheaper initially but require more custom transformation logic and generate higher maintenance costs over time.
For the full technical breakdown, see our guide to FHIR integration for healthcare apps.
3. Team Composition and Geography: $50–$250/hr Variance
US-based senior healthcare developers: $150–$250/hr. Eastern Europe and India senior healthcare developers: $50–$100/hr. For a 2,000-hour project, the rate difference is $200,000–$300,000. That looks like an obvious decision until you factor in domain experience.
A team without prior HIPAA implementation experience spends 30–40% more time on compliance architecture than a team that has built compliant systems before. A developer encountering HL7v2 message formats for the first time takes three times longer to build a working EHR integration than one who has done it, according to analysis from Interexy. The savings from lower hourly rates disappear entirely in additional hours and rework cycles.
The right evaluation is not hourly rate. It is: has this team built HIPAA-compliant apps before? Have they integrated with the specific EHR system on your list? Do they have active developer program memberships with Epic or Cerner that eliminate certification queue time? Those questions determine actual total cost far more than the rate card.
4. Platform Choice: Native vs Cross-Platform Saves 30%
Building separate native iOS and Android apps costs roughly 1.8x a single-platform build. Cross-platform frameworks (Flutter, React Native) share a single codebase across both platforms, saving 30–40% for most patient-facing healthcare apps.
Cross-platform is the right choice for 80% of healthcare apps: patient portals, telemedicine interfaces, wellness apps, medication management, RPM patient-facing apps. Choose native when you need low-level hardware access: direct Bluetooth stack communication for medical device connectivity, biometric authentication beyond what standard SDKs expose, or maximum performance for imaging applications.
The common mistake is defaulting to native "because it is better" without evaluating what the additional 80% cost buys you in your specific use case.
5. Real-Time Infrastructure: $30K–$80K Added Cost
Any feature involving live data, telemedicine video, RPM vitals alerts, real-time secure messaging, live monitoring dashboards, requires backend infrastructure that standard request-response apps do not need:
WebSocket or server-sent event connections for live data streams
Event-driven architecture for alert triggering (vitals breach thresholds)
HIPAA-eligible video infrastructure (Twilio, Vonage, not Zoom)
Load testing and performance validation under concurrent user scenarios
Higher-tier cloud infrastructure with lower latency requirements
This is not a feature cost that shows up on one line of your scope document. It is an infrastructure investment that affects your database architecture, your DevOps setup, your cloud tier, and your QA strategy. Budget $30,000–$80,000 for a real-time layer, separate from feature development costs.
Hidden Costs That Blow Budgets Mid-Project
The four hidden costs that most frequently cause healthcare app budgets to overrun are annual penetration testing ($15K–$40K), legal review of BAAs and privacy documentation ($5K–$20K), EHR vendor certification queues that add weeks without warning, and clinical staff validation time that never appears on a vendor invoice but is a real organizational cost.
Annual penetration testing. Any clinical app sold to hospital systems or enterprise health plans requires independent penetration testing from a certified third-party auditor. The cost runs $15,000–$40,000 per engagement. Some hospital procurement contracts require quarterly testing. This is not optional and it is not in the initial build scope, it is an ongoing operating cost that must be in your year-one budget.
Legal review. Business Associate Agreements, Terms of Service, Privacy Policies, patient consent forms, and state-specific telehealth compliance documents all require legal review from healthcare-specialized attorneys. Healthcare legal specialists charge $300–$600/hr. Budget $5,000–$20,000 for initial legal work, more if you are operating across multiple states with varying telehealth regulations.
EHR vendor certification queues. Epic's App Orchard and Connection Hub review processes run 4–8 weeks. Cerner's review process has its own queue. These timelines are not under your control and they are not in your vendor's estimate. If you do not book sandbox access and certification reviews during the discovery phase, you discover the queue mid-project while your sprint velocity has already been planned against a timeline that assumed no wait.
Clinical staff validation time. Your physicians, nurses, or clinical informatics team will spend time reviewing workflows, testing edge cases, and providing feedback on clinical logic. This typically runs 40–80 hours of senior clinical staff time per major review cycle. It does not appear on anyone's invoice. But it is real time with real opportunity cost, and any project that assumes clinical validation "happens automatically" underestimates the coordination and scheduling involved.
The example that plays out repeatedly: a project scoped at $175,000 reaches $265,000 because the EHR certification added eight weeks of idle time billed at maintenance rates, the penetration test was not in the budget, legal review ran $18,000 for a three-state telehealth product, and one round of clinical validation feedback required three sprint revisions to the care plan workflow.
How to Phase Your Build to Control Cost

The correct phasing for a healthcare app is: a paid discovery sprint to define compliance architecture and EHR integration scope (2–4 weeks, $15,000–$30,000), followed by an MVP covering the single core clinical workflow with HIPAA infrastructure in place (8–16 weeks, 40–60% of total budget), then Phase 2 adding integrations, secondary workflows, and advanced features.
The discovery sprint is not optional for healthcare. Architecture decisions made in the first four weeks of a project determine approximately 70% of total cost, according to Webkorps' AI healthcare app cost analysis. A proper discovery phase identifies $30,000–$100,000 in scope changes before they become $90,000–$300,000 mid-project rework items. The cost of discovery is always less than the cost of the architecture decisions it prevents.
The healthcare MVP definition differs from consumer app MVP. A healthcare MVP must include the full HIPAA compliance layer and at least read-only EHR access from sprint one. Stripping those as "Phase 2" is how budgets double: the compliance retrofit and EHR integration performed after the rest of the system is built is significantly more expensive than building them in.
Phase 1 (MVP): One core clinical workflow. Full HIPAA infrastructure. One EHR integration (read-only). Basic provider and patient UI. Core notification system. 40–60% of total budget.
Phase 2: Second EHR system. Bidirectional write-back. Advanced analytics. Secondary workflows. AI features if required. Remaining 40–60%.
Budget rule of thumb: add 25% contingency on your first clinical app build. If you have never integrated with the specific EHR vendor on your list, add another 15%.
For the full build process from concept to launch, see our guide to launching a healthtech app in under 90 days and our step-by-step guide to how to develop a healthcare app.
How to Build Without Cutting Compliance
The three most effective ways to reduce healthcare app development cost without compromising compliance are using established HIPAA-eligible third-party infrastructure instead of building it, choosing cross-platform over native for patient-facing apps, and working with a team that has existing EHR vendor developer relationships and certifications.
Do not build what already exists compliantly. Twilio and Vonage for HIPAA-eligible video. Stripe for healthcare payment processing. Auth0 or Okta for identity management and MFA. AWS or Azure for HIPAA-eligible hosting. These are not shortcuts, they are the industry standard. Using them instead of custom-building saves $40,000–$100,000 and eliminates the compliance risk of an untested custom implementation.
Choose cross-platform over native for any app where deep device hardware access is not required. For most patient-facing healthcare apps, it saves 30%.
Team experience with your specific EHR vendor matters more than hourly rate. A team with active Epic Connection Hub membership and prior certification history eliminates 4–8 weeks of queue time. At $80–$150/hr blended rate, that is $25,000–$60,000 in avoided delay cost.
One of the most common false economies is choosing staff augmentation over a managed team for clinical builds. Individual augmented developers do not produce HIPAA compliance documentation, sprint compliance logs, or architecture decision records as default outputs of their work. A managed pod builds these into the operating rhythm of every sprint. Our guide to what is a managed development team explains the ownership difference.
If you are evaluating whether to build in-house or partner, our guide to outsourcing healthcare product development covers the governance and accountability decisions involved.
Latent builds healthcare apps using managed pods, with HIPAA compliance, FHIR architecture, and sprint compliance documentation built in from day one. MVPs in 8–14 weeks, 100+ products shipped across 14 countries. Book a free 30-minute discovery call to get a realistic estimate for your specific product type.
Annual Operating Costs After Launch
Annual operating costs for a clinical healthcare app run 15–25% of initial development cost for maintenance, plus $5,000–$50,000/year for HIPAA-eligible cloud hosting, $15,000–$40,000 for annual penetration testing, and third-party API subscription fees. A $200,000 build typically costs $60,000–$100,000 per year to operate correctly.
Maintenance at 15–25% of build cost covers: security patches (critical for any app with PHI), OS updates (Apple and Google release major iOS/Android updates twice yearly and deprecate APIs), new device SDK versions for wearable integrations, EHR API version updates as vendors evolve their FHIR implementations, and compliance documentation updates as regulations change. This is not optional for clinical apps. An app that skips a security patch cycle is not just a technical liability, it is a HIPAA liability.
Cloud hosting on HIPAA-eligible infrastructure runs $500–$5,000/month depending on user load, data storage volume, and real-time infrastructure requirements. Standard cloud tiers do not include the BAA required for PHI. HIPAA-eligible tiers cost more and must be selected and configured deliberately.
Third-party API fees add up: Twilio video charges per minute of video, EHR marketplace fees apply if you list in Epic's App Orchard or Oracle's marketplace, analytics platforms charge by monthly active user. Budget $500–$5,000/month depending on usage patterns.
Total cost of ownership for a $200,000 clinical app: development ($200K) + Year 1 operating costs ($70K–$100K) + ongoing annual costs ($60K–$100K/year). This needs to be in the business case at the start, not discovered during the first budget review after launch.
What It Actually Costs to Build Secure and Right the First Time
The question framed wrong is: "What is the cheapest path to launch?"
The question framed right is: "What is the cost of a healthcare data breach ($10.22M US average in 2025), a failed hospital procurement process because compliance documentation was missing, or a six-sprint compliance retrofit, versus building it correctly in the first place?"
The teams that consistently bring healthcare products to market on budget are the ones that front-loaded the decisions: compliance architecture in discovery, EHR integration vendor relationships secured before development starts, and a team with prior experience on both. The teams that consistently double their budgets are the ones that deferred those decisions because the initial estimate looked cleaner without them.
Latent builds healthcare products using managed execution pods, cross-functional teams that own delivery from sprint planning through deployment, with HIPAA compliance, FHIR architecture, and IP documentation built into the operating rhythm from day one. We have shipped 100+ products across 14 countries, including telemedicine platforms, RPM systems, clinical apps, and patient engagement tools.
If you are scoping a healthcare app build and need a realistic, product-specific cost estimate, book a free 30-minute discovery call. We will map your product type, your compliance requirements, your EHR integration list, and give you a defensible budget range before you commit to anything.
Or start with a free 2-week discovery sprint: we scope the architecture, define the compliance path, and produce a full technical specification before your first dollar of development spend. Book your discovery sprint.
Frequently Asked Questions
How much does it cost to build a healthcare app in 2026?
Healthcare app development cost in 2026 ranges from $40,000–$80,000 for a wellness or fitness app with no clinical data, $80,000–$150,000 for a patient-facing portal with EHR access, $100,000–$200,000 for a telemedicine platform MVP, $150,000–$300,000 for a remote patient monitoring platform, $150,000–$300,000 for an AI clinical app MVP, and $200,000–$400,000+ for an enterprise clinical platform. The range is wide because the products are fundamentally different. A wellness tracker and a multi-EHR telemedicine platform share almost nothing cost-wise.
What is the most expensive part of healthcare app development?
EHR integration and HIPAA compliance architecture together typically account for 35–50% of total budget in clinical apps. A single EHR integration (read-only FHIR) starts at $15,000–$25,000; bidirectional integration with Epic starts at $50,000–$80,000. HIPAA compliance adds 20–30% to total budget. These two line items alone often exceed the total budget that founders initially allocate for the entire project.
How much does HIPAA compliance add to app development cost?
HIPAA compliance architecture adds 20–30% to total development budget when built correctly from the start: typically $15,000–$75,000 depending on app complexity. This covers HIPAA-eligible hosting, encryption, audit logging, access controls, and BAA management. Retrofitting HIPAA compliance after launch costs 2–3x more than building it in from the start, plus the risk exposure during the gap.
How long does it take to build a healthcare app?
Typical timelines for a production-ready MVP: wellness app 8–16 weeks, patient portal 12–20 weeks, mental health app 10–18 weeks, telemedicine platform 14–24 weeks, RPM platform 16–28 weeks, AI clinical app 16–32 weeks, enterprise clinical platform 20–40 weeks. These timelines assume the discovery sprint has been completed and EHR vendor sandbox access has been secured before development starts. Missing either adds weeks regardless of team velocity.
What are the annual operating costs for a healthcare app?
Annual operating costs for a clinical healthcare app run 15–25% of initial development cost for maintenance and updates, plus HIPAA-eligible cloud hosting ($500–$5,000/month), annual penetration testing ($15,000–$40,000), and third-party API fees ($500–$5,000/month depending on usage). A $200,000 build typically costs $60,000–$100,000 per year to operate correctly. This figure must be in the business case from the start, not discovered after launch.

Chinmay Chandgude is a partner at Latent with over 9 years of experience in building custom digital platforms for healthcare and finance sectors. He focuses on creating scalable and secure web and mobile applications to drive technological transformation. Based in Pune, India, Chinmay is passionate about delivering user-centric solutions that improve efficiency and reduce costs.
Related Posts
Free MVP Architecture
Share your product idea — we'll design your MVP architecture for free, no commitment required. If it's a good fit, we'll show you what building it looks like.



